Endotoxin and Other Microbial Translocation Markers in the Blood: A Clue to Understand Leaky Gut Syndrome
Hiroshi Fukui
DOI10.21767/2573-5365.100023
Hiroshi Fukui*
Department of Gastroenterology, Endocrinology and Metabolism, Nara Medical University, 840 Shijo-Cho Kashihara, Nara, Japan
- *Corresponding Author:
- Hiroshi Fukui
Department of Gastroenterology, Endocrinology and Metabolism, Nara Medical University, 840 Shijo- Cho Kashihara, 634-8522 Nara, Japan
Tel: 81744223051
E-mail: hfukui@naramed-u.ac.jp
Received date: October 18, 2016; Accepted date: November 29, 2016; Published date: December 05, 2016
Citation: Fukui H. Endotoxin and other microbial translocation markers in the blood: A clue to understand leaky gut syndrome. Cell Mol Med 2016, 2:3.
Abstract
Gut affects various systems in the human body. The leaky gut hypothesis tells us that gut microbial products cause systemic low-grade inflammation, which enhances the progression of various human diseases. Microbial translocation attributable to intestinal barrier dysfunction and hyperpermeability have been proven in major human diseases. Among these microbial products, endotoxin/ lipopolysaccharide is most extensively studied in clinical situations. However, its detection in the blood and its impact in the clinical course still arouse much discussion. Overviewing the long-standing controversies in the assay system and the main results in various clinical situations, this review regards plasma endotoxin level as a feasible microbial translocation marker. Although the detection of bacterial DNA in the blood has been gradually accepted among other microbial products, uniformity of analytical methods and usefulness in the clinical site should be established. The results on peptidoglycan, flagellin, lipoteichoic acid, and (1→ 3)-β-D-glucan in the blood are still scarce. The analysis of Toll-like receptors has suggested that several microbial products act concomitantly as pathogen-associated molecular patterns (PAMPs) in the progression of various diseases. Collective efforts to read the whole story on leaky gut and its sequences from the side of circulating microbial products may lead future progress both in patient’s care and preventive medicine.
Abstract
Gut affects various systems in the human body. The leaky gut hypothesis tells us that gut microbial products cause systemic low-grade inflammation, which enhances the progression of various human diseases. Microbial translocation attributable to intestinal barrier dysfunction and hyperpermeability have been proven in major human diseases. Among these microbial products, endotoxin/ lipopolysaccharide is most extensively studied in clinical situations. However, its detection in the blood and its impact in the clinical course still arouse much discussion. Overviewing the long-standing controversies in the assay system and the main results in various clinical situations, this review regards plasma endotoxin level as a feasible microbial translocation marker. Although the detection of bacterial DNA in the blood has been gradually accepted among other microbial products, uniformity of analytical methods and usefulness in the clinical site should be established. The results on peptidoglycan, flagellin, lipoteichoic acid, and (1→ 3)-β-D-glucan in the blood are still scarce. The analysis of Toll-like receptors has suggested that several microbial products act concomitantly as pathogen-associated molecular patterns (PAMPs) in the progression of various diseases. Collective efforts to read the whole story on leaky gut and its sequences from the side of circulating microbial products may lead future progress both in patient’s care and preventive medicine.
Keywords
Endotoxin; Bacterial DNA; Peptidoglycan; Flagellin; Lipoteichoic acid; (1→3)-β-D-glucan; Microbial translocation; Leaky gut; Toll-like receptors
Introduction
Pathogenic roles of gut and gut dysbiosis have been proposed in various human diseases. The passage of viable bacteria from the intestinal lumen through the mesenteric lymph nodes and other sites are defined as bacterial translocation (BT). The concept of BT was later broadened to microbial products or their fragments, such as endotoxin, peptidoglycan, lipopeptides, and bacterial DNA [1]. On the other side, intestinal epithelial barrier dysfunction and increased permeability have been described in various human diseases, such as inflammatory bowel disease (IBD) [2-7], irritable bowel syndrome [8,9] alcoholic liver disease [10-13] nonalcoholic steatohepatitis (NASH) [14,15] liver cirrhosis [16-19], primary biliary cholangitis (PBC) [20], acute pancreatitis [21-23], type 1 and type 2 diabetes [24-27], chronic kidney disease [28-30], chronic heart failure (CHF) [31,32] and depression [33,34]. Detrix et al. [35] has focused on the delicate role of gut mucosal interface in patients with various surgical or traumatic insults. In general, the leaky gut hypothesis explains that the intestinal barrier dysfunction provokes the chronic low-grade inflammation and functional disturbances in various target organs in virtue of microbial products, which play major roles in the development and progression of these diseases [36]. Several useful markers of gut wall integrity have been proposed. Intestinal fatty acid binding protein (I-FABP), primarily limited to mature enterocytes of the small and large intestine, is a plasma/ urinary marker for early enterocyte cell death [35]. It rises rapidly after episodes of acute intestinal ischemia and inflammation [35]. Measurement of tight junction (TJ) proteins such as claudin-3 in the urine and zonulin levels in the blood reflect the dysfunction of TJ causing leaky gut [35-37]. Increased level of D-lactate, a product of bacterial fermentation, is correlated with bacterial overgrowth, short bowel syndrome, and mesenteric ischaemia [35]. Plasma Dlactate was high in patients with end-stage renal disease and positive blood bacterial DNA [38].
The microbial products are translocated from the intestinal lumen to the circulation through disrupted TJs. They react to toll-like receptors (TLRs) in the macrophages, lymphocytes and variable cells and induce inflammation in various tissues. Each TLR detects a specific pathogen-associated molecular pattern (PAMP), including endotoxin/lipopolysaccharide (detected by TLR4), bacterial lipoprotein and peptidoglycan (detected by TLR2), flagellin (detected by TLR5), unmethylated CpG DNA (detected by TLR9), double-stranded RNA (detected by TLR3), and single-stranded RNA (detected by TLR7 and 8). TLR1 and TLR6 recognize tri-acyl lipopeptides and di-acyl lipopeptides, respectively, in cooperation with TLR2 [39,40]. Endotoxin binds to TLR4 with co-receptor CD14 and MD-2. TLR2 heterodimerizes with TLR1 or TLR6 to recognize lipoprotein and peptidoglycan derived from Gram-positive bacteria [41]. Intracellular TLR3 and TLR9 are activated by microbe-derived nucleic acids including double stranded RNA and CpG motif containing unmethylated DNA, respectively [41]. Taken together, TLRs 1, 2, 4, 5 and 6 seem to specialize in recognizing mainly bacterial products, whereas TLRs 3, 7 and 8 seem to specialize in viral detection [40]. TLR 9 are related both of them.
The levels of these PAMPs in the blood are increased in various clinical situations. Although endotoxin is the most popular circulating marker reflecting gut microbial translocation, the detection of circulating endotoxin is still not complete with several methodological difficulties [1]. Other microbial products have not yet been established as universal inflammatory mediators in the blood. We should reconsider the assay method of these substances and evaluate their relationships to intestinal permeability, leaky gut markers, and pro-inflammatory cytokine and chemokines before we admit them as gut-derived inflammatory mediators with pathogenic relevance in the leaky gut syndrome.
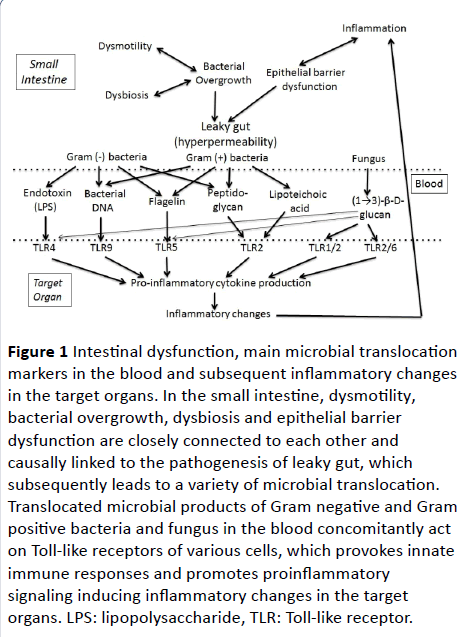
This review will focus on these microbial products as translocation markers and inflammatory moderators in relation to gut leakiness and various inflammatory changes to understand the concept of leaky gut syndrome and to find out whether they are useful circulating markers reflecting gutderived inflammatory changes. Figure 1 summarized the intestinal dysfunction, main microbial translocation markers in the blood and subsequent inflammatory changes in the target organs.
Figure 1 Intestinal dysfunction, main microbial translocation markers in the blood and subsequent inflammatory changes in the target organs. In the small intestine, dysmotility, bacterial overgrowth, dysbiosis and epithelial barrier dysfunction are closely connected to each other and causally linked to the pathogenesis of leaky gut, which subsequently leads to a variety of microbial translocation. Translocated microbial products of Gram negative and Gram positive bacteria and fungus in the blood concomitantly act on Toll-like receptors of various cells, which provokes innate immune responses and promotes proinflammatory signaling inducing inflammatory changes in the target organs. LPS: lipopolysaccharide, TLR: Toll-like receptor.
Endotoxin and Related Markers
History of blood endotoxin assay and their problems
Lipopolysaccharide (LPS) known as endotoxin is a major component of the Gram-negative bacterial wall. It can cross the deranged paracellular TJ or can be taken up by the enterocytes coupled with damaging lipoproteins, because it has a strong affinity for chylomicrons [42,43]. Its detection in the blood has a long and evolving history but is still not complete with several methodological difficulties 1. Endotoxemia was first demonstrated by the Limulus amoebocyte lysate (LAL) test and later by several quantitative assays, such as the chromogenic Limulus assay and the turbidometric endotoxin assay. Although these assays have been shown to give reliable results for minute amount of endotoxin in water, measurements of endotoxin in blood present some difficulties. Major problems include the way of preparing standard curves [43-45], the optimal method for eliminating plasma inhibitors of endotoxin [45-47], and specificity of LAL for endotoxin [48,49]. We have insisted that a standard curve should be prepared for each individual plasma sample in the endotoxin determination, because ideal 100% recovery of endotoxin is not validated in any trial of plasma pretreatment [45]. The internal standard is especially necessary in the acid pretreatment, where strict adjustment of pH (i.e. neutralization) for the chromogenic assay is sometimes difficult [50,51]. However, the influence of slight pH shift can be overcome by the existence of internal standard. We discovered hidden extra portion of endotoxin in plasma of patients with chronic liver diseases, using new way of plasma pretreatment either by Tween 80 in the dilution and heating method or by triethylamine in the perchloric acid method [50]. Finally, the LAL reagents widely used in the world react not only endotoxin but also (1,3)-β-D-glucan, component of cell wall of fungus [48], because they contain factor G reacting (1,3)-β-D-glucan in addition to factor C reacting endotoxin. Although endotoxin-specific reagents were produced early in Japan by removing G-factor from the lysate 48, proposed methods of sample pretreatment thereafter [52-54] were not adequate for the detection of minute amount of endotoxin in the blood of patients without bacteremia. Although some Japanese investigators have doubted the existence of portal endotoxemia, spillover endotoxemia or metabolic endotoxemia because of the negative results in their studies using the endotoxin-specific LAL tests, I disagree with them because we did detect endotoxemia in patients with chronic liver diseases by our improved chromogenic assay using endotoxin-specific substrate Endospecy (Seikagaku Kogyo Co., Tokyo, Japan) after the pretreatment of sample by perchloric acid and triethylamine [49-51]. A final pH of the sample was always adjusted to 7 by careful titration of triethylamine and the reactivity of each sample containing internal standard was confirmed by kinetic analysis [51]. The results of our measurement of plasma endotoxin in 90 patients with liver cirrhosis and 11 patients with chronic hepatitis with this method were summarized as follows: 1) There was an increase of plasma endotoxin with the progression of chronic liver disease. 2) In patients with bleeding from esophageal varices, plasma endotoxin increased for 3 days after the bleeding and thereafter decreased. 3) Endotoxin level increased as the progression of Child-Pugh grades and was negatively correlated to prothrombin time [1,49]. However, this improved method has not been generally accepted because of its methodological complexity despite its precise setting and reliability for plasma endotoxin assay. The prevailing endotoxin-specific turbidometric assay also has a drawback of poor sensitivity for the clinical use. Obata et al. [55] developed a new detection method using laser scattering photometry to analyze the formation of small particles of clotted enzyme in the process of LAL gelation. This endotoxin scattering photometry (ESP) has been proved to be more sensitive than the conventional turbidimetric LAL assay and proposed to be useful in discriminating between sepsis and septic shock in patients undergoing gastrointestinal emergency surgery [56].
Significance of endotoxemia in various diseases
Most studies on endotoxin measurement in the world have used non-specific LAL reagents after the dilution and heating of samples, ignoring the above problems. There still remains various problems on the overall assay validation as described in a recent extensive review [57]. However, accumulating results on clinical endotoxemia tested by this simple modification of LAL test are generally acceptable for clinicians, because they reflected clinical findings well and were closely associated with inflammatory reactions in various diseases. I would like to list up positive results in relation to leaky gut hypothesis in various diseases.
Endotoxemia in liver diseases: Among all liver diseases, alcoholic liver injury has been admitted as the typical entity in close association with leaky gut and endotoxemia. There is strong evidence to support the concept that gut-derived endotoxin plays a central role in the initiation and progression of alcohol-induced liver injury [58]. Once endotoxin reaches various organs, it powerfully stimulates TLR4 both in hepatic macrophages (Kupffer cells) and extrahepatic macrophages, which activate downstream signalling pathways responsible for overproduction of pro-inflammatory cytokines such as TNF- α, IL-6, and IL-8. Plasma endotoxin levels were increased with the progression of alcoholic liver injury and reached the maximal level in patients with alcoholic cirrhosis and severe alcoholic hepatitis who showed marked hypercytokinemia [59]. Plasma endotoxin level was reported to be positively correlated to TNF-α [60] and IL-8 levels [59]. Parlesak et al. [12] further found significant correlation between the plasma endotoxin levels and the intestinal permeability measured by the PEG Mr 4000 method.
In patients with cirrhosis, the plasma endotoxin levels progressively increased in relation to the severity of liver dysfunction [49,61]. Lumsden et al. [62] and Tachiyama et al. [63] further found significant increase of endotoxin levels in the portal blood from cirrhotic patients. This suggested an increased intestinal production and/or absorption of endotoxin in cirrhotics, which later opened the discussion on bacterial overgrowth and leaky gut in liver cirrhosis. Major complications of liver cirrhosis such as renal disturbance [64,65] gastrointestinal bleeding [51,65,66] and infection are reported to be related to endotoxemia. Recently TJ proteins occluding and claudin-1 expression were reported to be inversely correlated to endotoxin levels, which suggests that altered intestinal TJ expression leads to intestinal hyperpermeability and endotoxemia in liver cirrhosis [67].
Significant endotoxemia was also detected in patients with early stage of primary biliary cholangitis (PBC), and increased immunohistochemical expression of TLR4 and CD14 was found in the liver of PBC patients [68].
Recent clinical studies have brought the attention of clinicians to the role of endotoxemia in patients with nonalcoholic fatty liver disease (NAFLD), the hepatic manifestation of the metabolic syndrome. NAFLD includes a spectrum of pathological changes ranging from the simple fatty liver (NAFL), nonalcoholic steatohepatitis (NASH) to fibrosis and cirrhosis [69]. NAFLD patients reveal gut hyperpermeability characterized by disruption of the intercellular TJs with decreased ZO-1 expression, which may enhance translocations of bacteria and their products [14]. Several groups reported elevated serum endotoxin in NAFLD and NASH patients [70-72]. NASH patients showed endotoxemia and overexpression of TLR4 in the liver [73,74] associated with pro-inflammatory cytokine production and inflammation. Elevated endotoxin level was further correlated with insulin resistance and several inflammatory cytokines in NAFLD patients [75,76]. NAFLD patients with small intestinal bacterial overgrowth (SIBO) showed significantly higher endotoxin levels and TLR4 expression in the liver [74].
Serum lipopolysaccharide-binding protein (LBP), which has longer half-life than endotoxin, is evaluated as another useful surrogate marker of BT and endotoxemia [76]. LBP levels were associated with pro-inflammatory state and hemodynamic derangement in liver cirrhosis, which were proved to be mitigated by selective intestinal decontamination with norfloxacin [77]. In non-infected cirrhotics with ascites, increased serum LBP was selected as the only factor independently associated with first severe bacterial infection in a multivariate analysis [78].
Metabolic endotoxemia: In type 2 diabetes together with metabolic syndrome, the gut barrier dysfunction is again considered to induce BT and so-called metabolic endotoxemia, which subsequently predispose to systemic low-grade inflammation and insulin resistance [79]. Increased intestinal permeability and its relation to systemic inflammatory markers were reported in these patients [27]. Although baseline endotoxin level was already high in patients with type 2 diabetes [80,81], high-fat meal further augmented this endotoxemia [81]. Hawkesworth et al. [82] reported that endotoxin levels were highest in the obese-diabetic women compared with the obese non-diabetic and lean women. On the contrary, anti-core endotoxin IgM antibody (EndoCab IgM) levels were markedly lower in the obese and obese diabetic women compared with their lean counterparts. This could be explained by degradation of IgM-LPS complex that constantly neutralizes a persistent endotoxin leakage from the gut [82]. In type 2 diabetes, endotoxin activity was further positively correlated with the serum levels of TJ protein ZO-1 and proinflammatory TNF-α and IL-6 [83]. In the feces of type 2 diabetics, relatively higher abundance in endotoxin producing Gram-negative bacteria and lower abundance in butyrateproducing bacteria were reported [84].
Endotoxemia in inflammatory bowel diseases: The relation of endotoxemia to active Crohn’s disease (CD) was noted early in the period of LAL test [85,86]. Gardiner et al. [87] found endotoxemia in 88% patients with ulcerative colitis (UC) and 94% patients with CD even during clinical relapse and that endotoxemia was correlated with anatomic extent and clinical activity of UC. They further showed that plasma IgG endotoxin core antibody concentrations were significantly high in patients with CD, highest in patients with small intestinal CD, and correlated with endotoxemia and the soluble TNF receptor p55 [87]. They concluded that endotoxemia and its correlation with disease activity, disease extent, and circulating TNF supported a pathogenic role of endotoxin in IBD [87]. Pastor Rojo et al. [88] later found the elevation of plasma endotoxin levels in 48% patients with CD and in 28% patients with UC, where endotoxin, LBP and sCD14 levels were correlated with disease activity and normalized after treatment. Lakatos et al. [89] further reported that LBP and sCD14 levels were significantly correlated to high-sensitivity C-reactive protein (hs-CRP) and admitted that they were useful markers of active disease like hs-CRP.
Endotoxemia in pancreaticobiliary diseases: Endotoxemia was found in 51%~85% patients with severe acute pancreatitis [90,91] and was more common in non-survivors compared with survivors [90]. Necrotizing pancreatitis is accompanied by persistent marked endotoxemia [92]. The presence of endotoxin in blood and peritoneal fluid was associated with the disease severity, systemic complications, and mortality rates of acute pancreatitis [93]. EndoCab IgM levels conversely decreased early in patients with severe acute pancreatitis, although it remained relatively unchanged in those with mild pancreatitis [91,94,95]. In patients with acute pancreatitis, intestinal permeability was proved to be increased [21-23] which was correlated with plasma endotoxin [21-23,96] serum TNF-α [21,23] IL-6, and CRP levels and with the severity index estimated by computed tomography [23]. Mucosal function was injured early in those with organ dysfunction [21]. The expression of TJPs (occludin and ZO-1) in the colonic mucosal tissue was decreased in patients with severe acute pancreatitis, 62% of which showed BT (positive bacterial DNA in the peripheral blood) [97]. It is thus plausible that the failure of intestinal barrier predisposes to translocation of bacteria and inflammatory products through the intestinal wall, which can induce the infection of necrotic pancreas and systemic inflammatory response [98]. Plasma endotoxin was positively correlated with the abundance of Enterococcus, whereas serum IL-6 levels were positively correlated with the abundance of Enterobacteriaceae and Enterococcus and negatively correlated with that of Bifidobacterium in the feces, which suggested that the intestinal dysbiosis may be involved in endotoxemia and inflammation of acute pancreatitis [99].
The relation between obstructive jaundice and endotoxin was detected early in 1976, when Bailey [100] detected endotoxemia in 67% of portal blood and 54% of peripheral venous blood from patients with obstructive jaundice and thought that this endotoxemia was mostly gut-origin. He additionally noted that patients with endotoxemia showed evident decrease in endogenous creatinine clearance postoperatively, while those without endotoxemia did not [100]. The following studies further confirmed that malignant obstructive jaundice caused endotoxemia and inflammatory cytokinemia [101,102]. Several authors [101,103,104] reported increased intestinal permeability, which was also associated with BT [105,106]. Altered TJP, decreased expression of occluding, claudin-1 and -7, was further found in the duodenal epithelium of patients with obstructive jaundice [106]. The significance of endotoxemia as a key mediator of obstructive jaundice was thus established by the LAL test and its modification. Nevertheless, Kimmings et al. [106] reported that baseline plasma endotoxin levels in patients with obstructive jaundice were unexpectedly low and were not affected by the biliary drainage, while increased endotoxin binding proteins (LBP, sCD14 and BPI) were reduced after the drainage. As they stated, the endotoxin assay is potentially influenced by the yellow color of jaundiced plasma [101]. Other methods (i.e. turbidimetric assay or endotoxin acitivity assay) may solve this problem in jaundiced patients.
Endotoxemia in cardiorenal diseases: Plasma endotoxin and inflammatory cytokine levels were elevated in patients with CHF [107,108] and in adult patients with congenital heart disease [109], which were related to cardiac functional status. Increased intestinal permeability was again reported in patients with CHF [31]. These results suggest that disturbed intestinal microcirculation may induce gut barrier dysfunction and translocations of bacteria and their products, which may predispose to cytokine generation, thereby contributing to further impairment of cardiac function [110].
In the early 1980s [111,112] intestinal mucosal changes such as shortening of the villi, elongation of the crypts, and infiltration of lamina propria was reported in patients with chronic kidney disease (CKD). Intestinal hyperpermeability was reported later in these patients [28]. Recent quantitative endotoxin assay further revealed that circulating endotoxin levels were elevated along with the progression of CKD stages and serum CRP levels [113-115]. Vaziri et al. found marked disintegration of the colonic epithelial barrier structure and significant colonic dysbiosis in patients with advanced CKD [116] and concluded that this disruption of the intestinal epithelial barrier can induce systemic inflammation by enabling influx of endotoxin and other noxious luminal contents [117].
Other Microbial Translocation Markers
Peptidoglycan and flagellin
Peptidoglycan and flagellin, which bind to TLR2 and TLR5, respectively, have been implicated in the pathogenesis of inflammation of the liver and intestine [118]. Peptidoglycan is a common component of both Gram-positive and Gramnegative bacteria, accounting for about 70% and 20% of bacterial cell walls, respectively [119]. The silkworm larvae plasma (SLP) test was developed as a quantitative assay for peptidoglycan and β-glucan in plasma and dialysate [119,120]. Elevated SLP activity, which was noted in experimental hemorrhagic shock and alcohol intoxication [121,122], was reported also in infected patients during the postoperative period of gastrointestinal surgery [123]. It was also elevated in 83.6% patients with severe bacterial infection [119]. Transient rise of SLP activity noted in patients at the termination of cardiopulmonary bypass is considered attributable to hypoperfusion of small intestinal mucosa and resultant BT [124]. Kim et al. later developed a new tool to detect circulating peptidoglycan-like structure using a NOD2- transfected cell line and reported elevated levels of circulating NOD2 agonist in 90.5% patients with abdominal aortic surgery [125]. This circulating NOD2 agonist levels were correlated to IL-10 and cortisol levels and were more sensitive as a marker of BT than plasma endotoxin levels [125]. However, the measurement of peptidoglycan has been adopted by restricted surgical institutions, which makes its evaluation as a general BT marker difficult.
Flagellin is a monomeric subunit of flagella found on motile bacteria [126]. It is detected by an ELISA that recognizes a broad array of Gram-negative flagellin [127]. Flagellin interacts with basolateral TLR5 on gut epithelial cells leading to the secretion of inflammatory cytokines and chemokines [128]. Serum flagellin was detected either with or without endotoxemia in adult patients with short bowel syndrome (SBS) [127]. Flagellin-specific serum IgM, IgA, and IgG levels were also markedly increased in these SBS patients [127]. Elevated serum IgA and IgG titers against flagellin derived from Escherichia coli and other commensal bacteria were found in some patients with CD as well [129-131], which was associated with an increased adaptive immune response to flagellin [129-131], immune dysregulation and gut barrier dysfunction [127]. In addition, the level of antibodies to flagellin in the blood was higher in patients with diarrhea-predominant irritable bowel syndrome [132]. Human immunodeficiency virus (HIV) infection induces depletion of mucosal CD4+ lymphocytes, which is linked to disruption of gut epithelial integrity and increased mucosal translocation of bacteria and their products from the intestinal lumen to the systemic circulation [133,134]. The levels of anti-flagellin antibodies were also used as a microbial translocation markers after the treatment in patients with HIV-infection [135]. Munukka et al. [136] found that the expression of bacterial flagellinrecognizing TLR5 in the adipose tissue was associated with liver fat content and insulin sensitivity in healthy women, while no such associations were found for LPS-recognizing TLR4 expression. Together with their experimental results, they thought that the adipose tissue TLR5 expression may promote liver fat content in humans [136]. The evaluations of flagellin and its antibodies as serum BT markers have been thus very limited until now. Further studies in different clinical situations are needed.
Lipoteichoic acid
Lipoteichoic acid (LTA) is a cell wall component exclusive to Gram-positive bacteria and is shed during bacterial replication and after antibiotic administration [137]. Although LTA is the functional equivalent to endotoxin from Gram-negative bacteria, they induced differential cytokine/chemokine release via effects distal to activation of NF-κB/AP-1 [137] via TLR2 cluster [138]. LTA, as well as peptidoglycan, is released spontaneously into the culture medium during growth of Gram-positive bacteria, which was enhanced by incubation with antibiotics [139]. Like endotoxin, HDL has the highest binding capacity for LTA in the blood [140]. A continuous redistribution of LTA primarily from HDL to LDL occurs under simulated physiological conditions, which suggests that lipid transport proteins recognize and process endotoxin and LTA in a similar fashion [140]. However, unlike endotoxin, circulating level of LTA has not been reported in relation to clinical inflammation. Histologically, LTA-containing mononuclear cells were frequently detected in the portal tracts, particularly around the bile ducts and in hepatic sinusoids in patients with primary biliary cholangitis (PBC) [141]. LTA was detected at the sites of inflammation around damaged bile ducts in the livers of PBC, and sera from PBC patients showed higher levels of anti-LTA titers compared with those from chronic hepatitis C patients or from healthy subjects [142].
(1→3)-β -D-glucan
(1→3)-β-D-glucan (BG) is a polysaccharide found in the cell wall of fungal organisms such as Aspergillus, Candida, and Pneumocystis [143]. BG is highly immunogenic. It activates macrophages, neutrophils, and T-cells and stimulates release of pro-inflammatory cytokines [143]. (1-3)-β-D-glucan powerfully co-stimulate cytokine production (IL-6/IL-8) induced by ligands for TLR1/2, TLR2/6, TLR4, and TLR5 [144]. Circulating BG is measured by the modification of quantitative LAL test: removal of bacterial endotoxin-sensitive factor C from the LAL reagent. So far, several specific tests for BG detection have been developed, namely Fungitell kit, FungitecG test, Wako BG assay and GKT-25M set. BG might be a useful indicator of gut mucosal barrier impairment [145]. Serum BG levels are increased in patients with active CD and positively correlated with the severity of the disease [146]. Higher blood BG levels were significantly related to higher global deficit scores in HIV-infected adults, reflecting worse neurocognitive performance among patients with suppressed viral loads [145]. Translocation of gut microbial products into the systemic circulation is likely an important driver of immune dysfunction and persistent inflammation in the pathogenesis of neurocognitive dysfunction during HIV-infection [145].
Bacterial DNA
The detection of bacterial DNA in the blood by polymerase chain reaction (PCR) is considered as a surrogate marker for the diagnosis of BT showing higher sensitivity than blood cultures and longer half-life than endotoxin [76]. DNA is extracted from blood and PCR techniques used to amplify genes from E. coli, Bacteroides fragilis and 16SrRNA found in many Gram-positive and Gram-negative bacteria [147,148].
TLR9 is activated by bacterial DNA containing unmethylated CpG-dinucleotides in a particular base context called CpGmotif [149]. Bacterial DNA is present in 39% of the portal venous blood sample and in 43% of hepatic venous blood sample, suggesting that no major hepatic elimination of bacterial DNA occurs in cirrhosis [150]. Bacterial-DNA induces a marked immune reaction in vivo in patients with advanced cirrhosis and ascites [151]. Presence of bacterial DNA is also associated with aggravation of peripheral vasodilation and with worsening of intrahepatic endothelial dysfunction [152]. Cirrhotic patients with translocation of bacterial DNA from Gram-positive microorganisms showed increased proinflammatory cytokine levels unrelated to endotoxin [153]. In this meaning, bacterial DNA seems to be superior to evaluate BT as a whole compared with endotoxin.
Ortiz et al. [154] demonstrated that the translocation of bacterial products into the blood of morbidly obese patients characterizes a subgroup of patients who are not able to reduce their systemic inflammatory cytokine levels after following a massive weight reduction protocol consisting of a fasting period followed by bariatric surgery. Their multivariate analyses revealed bacterial DNA as an independent significant factor, explaining the systemic cytokine response and the insulin resistance levels [154].
Bacterial DNA was also found in 44% of patients with active CD versus 23% of patients with remitting disease [155]. Bacterial DNA in the blood was the only independent factor associated with relapse at 6 months by the multivariate analysis [155]. Preoperative bacterial DNA translocation into the blood increased the incidence of postoperative adverse outcomes in patients with CD who underwent abdominal surgery [156].
Gut bacterial DNA fragments are detectable in the bloodstream from both CKD and dialysis patients, and correlate with severity of systemic inflammation [30]. Circulating bacterial DNA fragment level is a strong predictor of cardiovascular event, need of hospitalization, as well as the progressive change in arterial stiffness in new peritoneal dialysis patients [157]. The plasma bacterial DNA level was also correlated with serum CRP and endotoxin levels in peritoneal dialysis patients [158]. In 20.7% of hemodialysis patients, bacterial DNA fragments were present in the whole blood. Serum CRP and IL-6 levels were significantly higher in chronic hemodialysis patients with bacterial DNA fragments than in those without [159].
The prevalence of positive bacterial DNA was significantly higher in HIV–infected patients with chronic hepatitis C than in healthy blood donors [160]. Patients with markers of advanced liver disease (F3/F4, and A2/A3) and high fibrosis progression rate (FPR >0.15) had higher plasma values of bacterial DNA than did patients without these markers of liver disease [160]. Surprisingly, Bala et al. [161] reported that a single alcohol binge (2 ml vodka 40% v/v ethanol/kg body weight in a total volume of 300 ml orange/strawberry juice) resulted in increased serum endotoxin and 16S bacterial rDNA levels in healthy individuals. This interesting observation further supports the usefulness of bacterial DNA as a marker of leaky gut.
In spite of these accumulating promising results, uniformity of analytical methods of bacterial DNA is still needed to ascertain its real value in routine clinical setting [76].
Table 1 summarized the changes in circulating microbial translocation markers in relation to expression of TLRs in various clinical situations. Several TLRs are sometimes concomitantly affected in aforementioned diseases. For example, hepatic TLR 1-5 mRNAs expression was upregulated in NAFLD patients [162]. Although TLR4 plays a cardinal role in the pathogenesis of alcoholic liver disease [163], upregulation of TLR3 and TLR7 in the liver tissue is associated with endstage alcoholic liver disease [164]. In alcohol-fed animals, most of hepatic TLRs expression (TLR1, TLR2, TLR4, TLR6, TLR7, TLR8 and TLR9) was further upregulated [165].
| LPS | Peptido glycan |
Flagellin | LTA | BG | Bact- DNA |
TLRs | |
|---|---|---|---|---|---|---|---|
| Alcoholic liver disease |
↑ | ↑ | Liver TLR3,4,7↑ | ||||
| Liver cirrhosis | ↑ | ↑ | PBMC TLR2,4↑ TLR4↓ recovered by antibiotics liver TLR2,4→↑ |
||||
| PBC | ↑ | anti-LTΑ↑ | Liver TLR3,4↑ | ||||
| NAFLD | ↑ | Liver TLR1-5↑ | |||||
| Severe obesity | ↑ | ↑ | Adipose tissue TLR2,3,4,5↑ |
||||
| Type 2 diabetes | ↑ | PBMC TLR2,4↑ adipose tissue TLR2,4↑ wounds TLR1,2,4,6↑ |
|||||
| Active Crohn’s disease |
↑ | anti-F (CBir-1)↑ |
↑ | ↑ | Colon epithelium TLR2,4↑ ileal epithelium TLR4↑ |
||
| Ulcerative colitis | ↑ | anti-F (CBir-1)↑ |
Colon epithelium TLR2,4↑ |
||||
| severe acute pancreatitis |
↑ | ||||||
| obstructive jaundice | ↑ | ||||||
| chronic heart failure |
↑ | Myocardium TLR4↑ |
|||||
| chronic kidney disease |
↑ | ↑ | PBMC TLR2,4↑ neutrophil TLR4↑ diabetic nephlopathy glomerular endothelium TLR2↑ tubular epithelium TLR4↑ |
||||
| Short bowel syndrome |
↑ | ↑ anti-F↑ |
|||||
| HIV-infection | ↑ | anti-F↑ | ↑ | ↑ | PBMC TLR6,7,8↑ advanced infection PBMC TLR2,3,4↑ |
||
| depression | anti- LPS↑ |
↑ | Brain TLR3,4↑ | ||||
| Cardiopulmonary bypass | ↑ | ↑ |
LPS: lipopolysaccharide (endotoxin), LTA :lipoteichoic acid, BG : (1→3)-β-D-glucan, anti-F: anti-flagellin, ↑: increased, ↓: decreased
Table 1 Changes in circulating microbial translocation markers in relation to expression of Toll-like receptors in various clinical situations.
TLRs expression in patients with liver cirrhosis are conflicting as summarized by Yang et al [166]. Although increased TLR4 expression in the peripheral blood mononuclear cells (PBMCs) was reported by one group [167], other investigators reported that TLR4 expression was decreased and TLR2 expression was increased in cirrhotic PBMC [168-170]. Testro et al. [171] noted that decreased TLR4 expression and hyporesponsiveness to LPS in PBMCs were recovered after antibiotics treatment targeting enteric Gram-negative bacteria in patients with advanced Child C alcoholic cirrhosis. In contrast, hepatic expression of TLR2 and TLR4 was increased or unchanged in patients with cirrhosis [166,168,172]. Soares et al. [172] thought that upregulation of TLR2, TLR4 and their proinflammatory mediators were associated with virus-induced hepatic inflammation-fibrosis-carcinoma sequence.
The Expression of TLRs in Various Diseases
In PBC patients, TLR3 is highly expressed on macrophages surrounding portal tract and hepatocytes [173], while TLR4 expression is significantly elevated in biliary epithelial cells, periportal hepatocytes [68], and PBMCs [174].
Colonic crypt epithelial cells isolated from active CD and ulcerative colitis revealed significantly higher expression of TLR2 and TLR4 compared with control cells [175]. Enhanced expression of TLR4 was also noted in crypt cells from ileal CD [175].
Type 2 diabetic subjects showed significantly increased TLR2, TLR4 mRNA and proteins in PBMCs [176]. As for diabetic complications, TLR1, 2, 4, and 6 mRNA expressions were increased significantly in wounds of diabetic patients compared with non-diabetic wounds [177]. Recent studies have further highlighted the critical role of TLRs, mainly TLR2 and TLR4, in the pathogenesis of diabetic nephropathy [178]. TLR2 and TLR4 are upregulated in monocytes, and TLR4 is upregulated in neutrophils of end-stage renal disease patients [179].
Chronic, untreated HIV-1 infection was significantly associated with increased mRNA expression of TLR6, TLR7, and TLR8 in PBMC and when analysis was limited to those with advanced disease (CD4 cell count <200 cells/ml) TLR2, TLR3, and TLR4 were additionally elevated [180]. In the postmortem brain of depressed suicide victims, TLR3 and TLR4 expressions were increased in the dorsolateral prefrontal cortex [181]. In case of cardiopulmonary bypass surgery, a 29% reduction in monocyte TLR4 expression was noted at the end of operation and more than 120% increase in monocyte TLR2 and TLR4 expression was noted in the following day [182].
Taken together, these results suggest that several microbial products might be concomitantly increased as pathogenassociated molecular patterns (PAMPs) and reacting to separate TLRs, which may work together and strongly promote the progression of major diseases. Although the additional effects of endogenous damage/danger-associated molecular patterns (DAMPs) unrelated to microbiome cannot be neglected especially in metabolic disorders such as NASH or type 2 diabetes, the whole figures of circulating PAMPs in clinical situations cannot be depicted at present.
In line with the leaky gut hypothesis, outlines of gut leakiness, endotoxin, TLRs and inflammatory mediators in various clinical situations were summarized also in my previous review [36].
Revisit to the Endotoxin Assay
The main issue of this article was to understand the concept of leaky gut syndrome from clinical microbial translocation markers. The detection of endotoxin in the blood is regarded as the most reliable tool for this purpose, although there still remain several problems in the methodology and the interpretation of results. We have previously compared endotoxin-specific chromogenic substrate with the conventional chromogenic substrate and could not find out any superiority of the endotoxin-specific test for evaluation of BT. Both tests were well correlated to clinical course and considered to be useful markers in patients with chronic liver diseases. It should be noted that (1-3)-β-D glucan powerfully co-stimulate cytokine production (IL-6/IL-8) induced by ligands for TLR1/2, TLR2/6, TLR4, and TLR5 [144]. Elevated plasma glucan levels in patients with bacterial infections and low plasma glucan levels in normal individuals may be attributable to the movement of glucan from the gut into the blood and not necessarily to the presence of pathogenic fungus [1,183]. Although most prevalent quantitative LAL test reacts (1-3)-β-Dglucan and is not endotoxin-specific, both endotoxin from Gram-negative bacteria and (1-3)-β-D-glucan from fungus are microbial translocation products [1] and strongly co-stimulate innate immune system and induce the production of inflammatory mediators. While the additive influence of (1-3)- β-D-glucan on the measured endotoxin level cannot be neglected, its close correlations to systemic inflammatory markers and clinical findings seems to validate the usefulness of the assay as a general marker of microbial translocation.
To confirm the usefulness of these assays, we can further try other new endotoxin assays and compare the results. Endotoxin activity assay [184] is an indirect method for evaluation of endotoxemia measuring the chemiluminescence of superoxide produced by neutrophils that incorporate endotoxin combined with anti-lipid A antibody and complements. This assay has been proved to be useful for assessing disease severity and predicting outcome in critically ill patients [185-187], liver transplant recipients [188] and patients with biliary tract infection [31]. We ourselves have noted its clinical usefulness for various hepatobiliary diseases (unpublished data). Its simplicity and rapidity may further broaden the potential clinical applications.
Two breakthroughs in the endotoxin assay, the factor C system [189] and the cell-based biosensor system [190,191], have been recently introduced, although they have not been intended to detect endotoxin in the blood. Both of them have a merit to protect horseshoe crab resources. If hTLR4A-MD2- CD14 cells reported by Jiang et al. [191] can be reconstituted for the detection of endotoxemia removing the interferences with responses by cytokines, this may become a promising alternative to endotoxin assay in the blood.
Conclusion
This review concludes that plasma endotoxin determination is considered as a feasible microbial translocation marker in spite of methodological controversies. Although the detection of bacterial DNA in the blood may be useful and promising, the detection method should be more simple and unified for routine clinical use. In order to determine an ideal setting of BT markers, we should continue further comprehensive studies on these and other microbial markers and their relations to host reactions. Our goal is to read the whole story on the leaky gut and its consequences in various clinical scene. Intestinal bacterial overgrowth and dysbiosis may additionally predispose to gut leakiness and BT. A rational attempt to modulate intestinal microbiome and permeability is a cornerstone for the prevention of pathological BT. The clinical approaches to the gut disturbances along with the leaky gut hypothesis appears to be a promising and innovative tool in controlling various diseases in the future.
Conflict of Interest
The author declares that there is no conflict of interest regarding the publication of this paper.
References
- Fukui H (2015) Gut-liver axis in liver cirrhosis: How to manage leaky gut and endotoxemia. World J Hepatol 7: 425-442.
- Wyatt J, Oberhuber G, Pongratz S, Puspok A, Moser G, et al. (1997) Increased gastric and intestinal permeability in patients with Crohn's disease. Am J Gastroenterol 92: 1891-1963.
- Oriishi T, Sata M, Toyonaga A, Sasaki E, Tanikawa K (1995) Evaluation of intestinal permeability in patients with inflammatory bowel disease using lactulose and measuring antibodies to lipid A. Gut 36: 891-896.
- Buning C, Geissler N, Prager M, Sturm A, Baumgart DC, et al. (2012) Increased small intestinal permeability in ulcerative colitis: Rather genetic than environmental and a risk factor for extensive disease? Inflamm Bowel Dis 18: 1932-1939.
- Gerova VA, Stoynov SG, Katsarov DS, Svinarov DA ( 2011) Increased intestinal permeability in inflammatory bowel diseases assessed by iohexol test. World J Gastroenterol 17: 2211-2215.
- Takaishi H, Matsuki T, Nakazawa A, Takada T, Kado S et al. (2008) Imbalance in intestinal microflora constitution could be involved in the pathogenesis of inflammatory bowel disease. Int J Med Microbiol 298: 463-472.
- Pitcher MC, Beatty ER, Cummings JH (2000) The contribution of sulphate reducing bacteria and 5-aminosalicylic acid to faecal sulphide in patients with ulcerative colitis. Gut 46: 64-72.
- Camilleri M, Lasch K, Zhou W (2012) Irritable bowel syndrome: methods, mechanisms, and pathophysiology. The confluence of increased permeability, inflammation, and pain in irritable bowel syndrome. Am J Physiol Gastrointest Liver Physiol 303: 775-785.
- Shulman RJ, Jarrett ME, Cain KC, Broussard EK, Heitkemper MM (2014) Associations among gut permeability, inflammatory markers, and symptoms in patients with irritable bowel syndrome. J Gastroenterol 49: 1467-1476.
- Bjarnason I, Peters TJ, Wise RJ (1984) The leaky gut of alcoholism: possible route of entry for toxic compounds. Lancet 1: 179-182.
- Keshavarzian A, Holmes EW, Patel M, Iber F, Fields JZ et al. (1999) Leaky gut in alcoholic cirrhosis: A possible mechanism for alcohol-induced liver damage. Am J Gastroenterol 94: 200-207.
- Parlesak A, Schafer C, Schutz T, Bode JC, Bode C (2000) Increased intestinal permeability to macromolecules and endotoxemia in patients with chronic alcohol abuse in different stages of alcohol-induced liver disease. J Hepatol 32:742-747.
- Leclercq S, Matamoros S, Cani PD, Neyrinck AM, Jamar F, et al. (2014) Intestinal permeability, gut-bacterial dysbiosis, and behavioral markers of alcohol-dependence severity. Proc Natl Acad Sci USA 111: 4485-4493.
- Miele L, Valenza V, La Torre G, Montalto M, Cammarota G, et al. (2009) Increased intestinal permeability and tight junction alterations in nonalcoholic fatty liver disease. Hepatology 49: 1877-1887.
- Giorgio V, Miele L, Principessa L, Ferretti F, Villa MP, et al. (2014) Intestinal permeability is increased in children with non-alcoholic fatty liver disease, and correlates with liver disease severity. Dig Liver Dis 46: 556-560.
- Campillo B, Pernet P, Bories PN, Richardet JP, Devanlay M, et al. (1999) Intestinal permeability in liver cirrhosis: relationship with severe septic complications. Eur J Gastroenterol Hepatol 11: 755-759.
- Pascual S, Such J, Esteban A, Zapater P, Casellas JA, et al. (2003) Intestinal permeability is increased in patients with advanced cirrhosis. Hepatogastroenterology 50: 1482-1486.
- Scarpellini E, Valenza V, Gabrielli M, Lauritano EC, Perotti G, et al. (2010) Intestinal permeability in cirrhotic patients with and without spontaneous bacterial peritonitis: is the ring closed? Am J Gastroenterol 105: 323-327.
- Pijls KE, Jonkers DM, Elamin EE, Masclee AA, Koek GH (2013) Intestinal epithelial barrier function in liver cirrhosis: an extensive review of the literature. Liver Int 33: 1457-1469.
- Feld JJ, Meddings J, Heathcote EJ (2006) Abnormal intestinal permeability in primary biliary cirrhosis. Dig Dis Sci 51: 1607-1613.
- Liu H, Li W, Wang X, Li J, Yu W (2008) Early gut mucosal dysfunction in patients with acute pancreatitis. Pancreas 36: 192-196.
- Ammori BJ, Leeder PC, King RF, Barclay GR, Martin, IG et al. (1999) Early increase in intestinal permeability in patients with severe acute pancreatitis: correlation with endotoxemia, organ failure, and mortality. J Gastrointest Surg 3: 252-262.
- Koh YY, Jeon WK, Cho YK, Kim HJ, Chung WG, et al. (2012) The effect of intestinal permeability and endotoxemia on the prognosis of acute pancreatitis. Gut Liver 6: 505-511.
- Damci T, Nuhoglu I, Devranoglu G, Osar Z, Demir M, et al. (2003) Increased intestinal permeability as a cause of fluctuating postprandial blood glucose levels in Type 1 diabetic patients. Eur J Clin Invest 33: 397-40.
- Bosi E, Molteni L, Radaelli MG, Folini L, Fermo I, et al. (2006) Increased intestinal permeability precedes clinical onset of type 1 diabetes. Diabetologia 49: 2824-2827.
- de Kort S, Keszthelyi D, Masclee AA (2011) Leaky gut and diabetes mellitus: what is the link? Obes Rev 12: 449-458.
- Horton F, Wright J, Smith L, Hinton PJ, Robertson MD (2014) Increased intestinal permeability to oral chromium (51 Cr) -EDTA in human Type 2 diabetes. Diabet Med 31: 559-563.
- Magnusson M, Magnusson KE, Sundqvist T, Denneberg T (1991) Impaired intestinal barrier function measured by differently sized polyethylene glycols in patients with chronic renal failure. Gut 32: 754-759.
- Wong J, Piceno YM, Desantis TZ, Pahl M, Andersen GL, et al. (2014) Expansion of urease- and uricase-containing, indole- and p-cresol-forming and contraction of short-chain fatty acid-producing intestinal microbiota in ESRD. Am J Nephrol 39: 230-237
- Lau WL, Kalantar-Zadeh K, Vaziri ND(2015) The gut as a source of inflammation in chronic kidney disease. Nephron 130: 92-98.
- Sandek A, Bauditz J, Swidsinski A, Buhner S, Weber-Eibel J, et al. (2007) Altered intestinal function in patients with chronic heart failure. J Am Coll Cardiol 50: 1561-1569.
- Pasini E, Aquilani R, Testa C, Baiardi P, Angioletti S, et al. (2015) Pathogenic gut flora in patients with chronic heart failure. JACC Heart Fail 4: 220-227.
- Kelly JR, Kennedy PJ, Cryan JF, Dinan TG, Clarke G, et al. (2015) Breaking down the barriers: the gut microbiome, intestinal permeability and stress-related psychiatric disorders. Front Cell Neurosci 9: 392.
- Naseribafrouei A, Hestad K, Avershina E, Sekelja M, Linlokken A, et al. (2014) Correlation between the human fecal microbiota and depression. Neurogastroenterol Motil 26: 1155-1162.
- Derikx JP, Luyer MD, Heineman E, Buurman WA (2010) Non-invasive markers of gut wall integrity in health and disease. World J Gastroenterol 16: 5272-52729.
- Fukui H (2016) Increased intestinal permeability and decreased barrier function: Does It really influence the risk of inflammation? Inflamm Intest Dis 1:in press.
- Moreno-Navarrete JM, Sabater M, Ortega F, Ricart W, Fernandez-Real JM (2012) Circulating zonulin, a marker of intestinal permeability, is increased in association with obesity-associated insulin resistance. PLoS One 7:e37160. 3356365
- Wang F, Jiang H, Shi K, Ren Y, Zhang P, et al. (2012) Gut bacterial translocation is associated with microinflammation in end-stage renal disease patients. Nephrology (Carlton) 17: 733-738.
- Omueti KO, Beyer JM, Johnson CM, Lyle EA, Tapping RI (2005) Domain exchange between human toll-like receptors 1 and 6 reveals a region required for lipopeptide discrimination. J Biol Chem 280: 36616-3625.
- Tsujimoto H, Ono S, Mochizuki H (2009) Role of translocation of pathogen-associated molecular patterns in sepsis. Dig Surg 26: 100-109.
- Seki E, Schnabl B (2012) Role of innate immunity and the microbiota in liver fibrosis: crosstalk between the liver and gut. J Physiol 590: 447-458.
- Piya MK, Harte AL, McTernan PG (2013) Metabolic endotoxaemia: Is it more than just a gut feeling? Curr Opin Lipidol 24: 78-85.
- Sturk A, Joop K, ten Cate JW, Thomas LL (1985) Optimalization of a chromogenic assay for endotoxin in blood. Prog Clin Biol Res 189: 117-137.
- Friberger P (1985) The design of a reliable endotoxin test. Prog Clin Biol Res 189: 139-149.
- Fukui H, Brauner B, Bode JC, Bode C (1989) Chromogenic endotoxin assay in plasma. Selection of plasma pretreatment and production of standard curves. J Clin Chem Clin Biochem 27: 941-946.
- Obayashi T (1984) Addition of perchloric acid to blood samples for colorimetric limulus test using chromogenic substrate: comparison with conventional procedures and clinical applications. J Lab Clin Med 104: 321-330.
- Tsuji K, Martin PA, Gaunnac GL (1987) Recovery of endotoxin from human plasma by acid oxidative treatments as monitored by an automated microtiter plate-chromogenic substrate Limulus amebocyte lysate (LAL) assay method. Prog Clin Biol Res 231: 443-457.
- Obayashi T, Tamura H, Tanaka S, Ohki M, Takahashi S, et al. (1985) A new chromogenic endotoxin-specific assay using recombined limulus coagulation enzymes and its clinical applications. Clin Chim Acta 149: 55-65.
- Fukui H, Tsujita S, Matsumoto M, Kitano H, Hoppou K, et al. (1998) Endotoxemia in chronic hepatitis and cirrhosis: Epiphenomenon or of pathological relevence? In: Blum H, Bode C, Bode JC, Sartor RB (Eds.). Gut and the Liver. Dordrecht, Boston, London: Kluwer Academic Publishers 251-262.
- Bode C, Fukui H, Bode JC (1993) "Hidden" endotoxin in plasma of patients with alcoholic liver disease. Eur J Gastroenterol Hepatol 5: 257-262.
- Fukui H, Matsumoto M, Tsujita S, Takaya A, Kojima H, et al. (1994) Plasma endotoxin concentration and endotoxin binding capacity of plasma acute phase proteins in cirrhotics with variceal bleeding: an analysis by new methods. J Gastroenterol Hepatol 9: 582-586.
- Inada K, Yoshida M, Takahashi T, Tamura S, Tanaka S, et al. (1990) A new perchloric acid treatment of human plasma for detection of endotoxin by an endotoxin-specific chromogenic test. Adv Exp Med Biol 256: 225-229.
- Tamura H, Tanaka S, Obayashi T, Yoshida M, Kawai T (1991) A new sensitive method for determining endotoxin in whole blood. Clin Chim Acta 200: 35-42.
- Tamura H, Tanaka S, Obayashi T, Yoshida M, Kawai T (1992) A new sensitive microplate assay of plasma endotoxin. J Clin Lab Anal 6: 232-238.
- Obata T, Nomura M, Kase Y, Sasaki H, Shirasawa Y (2008) Early detection of the Limulus amebocyte lysate reaction evoked by endotoxins. Anal Biochem 373: 281-286.
- Shimizu T, Obata T, Sonoda H, Akabori H, Miyake T, et al. (2013) Diagnostic potential of endotoxin scattering photometry for sepsis and septic shock. Shock 40: 504-511.
- Gnauck A, Lentle RG, Kruger MC (2016) Chasing a ghost?--Issues with the determination of circulating levels of endotoxin in human blood. Crit Rev Clin Lab Sci 53: 197-215.
- Yan AW, Fouts DE, Brandl J, Starkel P, Torralba M, et al. (2011) Enteric dysbiosis associated with a mouse model of alcoholic liver disease. Hepatology 53: 96-105.
- Fujimoto M, Uemura M, Nakatani Y, Tsujita S, Hoppo K, et al. (2000) Plasma endotoxin and serum cytokine levels in patients with alcoholic hepatitis: relation to severity of liver disturbance. Alcohol Clin Exp Res 24: 48S-54S.
- Hanck C, Rossol S, Bocker U, Tokus M, Singer MV (1998) Presence of plasma endotoxin is correlated with tumour necrosis factor receptor levels and disease activity in alcoholic cirrhosis. Alcohol Alcohol 33: 606-608.
- Lin RS, Lee FY, Lee SD, Tsai YT, Lin HC, et al. (1995) Endotoxemia in patients with chronic liver diseases: relationship to severity of liver diseases, presence of esophageal varices, and hyperdynamic circulation. J Hepatol 22: 165-72.
- Lumsden AB, Henderson JM, Kutner MH (1988) Endotoxin levels measured by a chromogenic assay in portal, hepatic and peripheral venous blood in patients with cirrhosis. Hepatology 8: 232-236.
- Tachiyama G, Sakon M, Kambayashi J, Iijima S, Tsujinaka T, et al. (1988) Endogenous endotoxemia in patients with liver cirrhosis--a quantitative analysis of endotoxin in portal and peripheral blood. Jpn J Surg 18: 403-408.
- Wilkinson SP, Moodie H, Stamatakis JD, Kakkar VV, Williams R (1979) Endotoxaemia and renal failure in cirrhosis and obstructive jaundice. Br Med J 2: 1415-1418.
- Clemente C, Bosch J, Rodes J, Arroyo V, Mas A, et al. (1977) Functional renal failure and haemorrhagic gastritis associated with endotoxaemia in cirrhosis. Gut 18: 556-560.
- Fukui H, Matsumoto M, Bode C, Bode JC, Tsujita S, et al. (1993) Endotoxaemia in patients with liver cirrhosis and upper gastrointestinal bleeding: detection by the chromogenic assay with plasma Tween 80 pretreatment. J Gastroenterol Hepatol 8: 577-581.
- Assimakopoulos SF, Tsamandas AC, Tsiaoussis GI, Karatza E, Triantos C, et al. (2012) Altered intestinal tight junctions' expression in patients with liver cirrhosis: a pathogenetic mechanism of intestinal hyperpermeability. Eur J Clin Invest 42: 439-446.
- Zhao J, Zhao S, Zhou G, Liang L, Guo X, et al. (2013) Altered biliary epithelial cell and monocyte responses to lipopolysaccharide as a TLR ligand in patients with primary biliary cirrhosis. Scand J Gastroenterol 46: 485-94.
- Fukui H (2015) Gut Microbiota and Host Reaction in Liver Diseases. Microorganisms 3: 759-791.
- Thuy S, Ladurner R, Volynets V, Wagner S, Strahl S, et al. (2008) Nonalcoholic fatty liver disease in humans is associated with increased plasma endotoxin and plasminogen activator inhibitor 1 concentrations and with fructose intake. J Nutr 138: 1452-1455.
- Harte AL, da Silva NF, Creely SJ, McGee KC, Billyard T, et al. (2010) Elevated endotoxin levels in non-alcoholic fatty liver disease. J Inflamm (Lond) 7: 15.
- Volynets V, Kuper MA, Strahl S, Maier IB, Spruss A, et al. (2012) Nutrition, intestinal permeability, and blood ethanol levels are altered in patients with nonalcoholic fatty liver disease (NAFLD). Dig Dis Sci 57: 1932-41.
- Alisi A, Manco M, Devito R, Piemonte F, Nobili V (2010) Endotoxin and plasminogen activator inhibitor-1 serum levels associated with nonalcoholic steatohepatitis in children. J Pediatr Gastroenterol Nutr 50: 645-649.
- Kapil S, Duseja A, Sharma BK, Singla B, Chakraborti A, et al. (2016) Small intestinal bacterial overgrowth and toll-like receptor signaling in patients with non-alcoholic fatty liver disease. J Gastroenterol Hepatol 31: 213-221.
- Jin R, Willment A, Patel SS, Sun X, Song M, et al. (2014) Fructose induced endotoxemia in pediatric nonalcoholic Fatty liver disease. Int J Hepatol 2014:560620.
- Bellot P, Frances R, Such J (2013) Pathological bacterial translocation in cirrhosis: pathophysiology, diagnosis and clinical implications. Liver Int 33:31-39.
- Albillos A, de la Hera A, Gonzalez M, Moya JL, Calleja JL, et al. (2003) Increased lipopolysaccharide binding protein in cirrhotic patients with marked immune and hemodynamic derangement. Hepatology 37:208-217.
- Albillos A, de-la-Hera A, Alvarez-Mon M (2004) Serum lipopolysaccharide-binding protein prediction of severe bacterial infection in cirrhotic patients with ascites. Lancet 363: 1608-1610.
- Festi D, Schiumerini R, Eusebi LH, Marasco G, Taddia M, et al. (2014) Gut microbiota and metabolic syndrome. World J Gastroenterol 20:16079-1609480.
- Pussinen PJ, Havulinna AS, Lehto M, Sundvall J, Salomaa V (2011) Endotoxemia is associated with an increased risk of incident diabetes. Diabetes Care 34: 392-407.
- Harte AL, Varma MC, Tripathi G, McGee KC, Al-Daghri NM, et al. (2012) High fat intake leads to acute postprandial exposure to circulating endotoxin in type 2 diabetic subjects. Diabetes Care 35: 375-382.
- Hawkesworth S, Moore SE, Fulford AJ, Barclay GR, Darboe AA, et al. (2013) Evidence for metabolic endotoxemia in obese and diabetic Gambian women. Nutr Diabetes 3: e83.
- Jayashree B, Bibin YS, Prabhu D, Shanthirani CS, Gokulakrishnan K, et al. (2014) Increased circulatory levels of lipopolysaccharide (LPS) and zonulin signify novel biomarkers of proinflammation in patients with type 2 diabetes. Mol Cell Biochem 388:203-210.
- Larsen N, Vogensen FK, van den Berg FW, Nielsen DS, Andreasen AS, et al. (2010) Gut microbiota in human adults with type 2 diabetes differs from non-diabetic adults. PLoS One 5: e9085.
- Aoki K (1978) A study of endotoxemia in ulcerative colitis and Crohn's disease. II. Experimental study. Acta Med Okayama 32: 207-216.
- Wellmann W, Fink PC, Benner F, Schmidt FW (1986) Endotoxaemia in active Crohn's disease. Treatment with whole gut irrigation and 5-aminosalicylic acid. Gut 27: 814-820.
- Gardiner KR, Halliday MI, Barclay GR, Milne L, Brown D, et al. (1995) Significance of systemic endotoxaemia in inflammatory bowel disease. Gut 36: 897-901.
- Pastor Rojo O, Lopez San Roman A, Albeniz Arbizu E, de la Hera Martinez A, Ripoll Sevillano E, et al. (2007) Serum lipopolysaccharide-binding protein in endotoxemic patients with inflammatory bowel disease. Inflamm Bowel Dis 13: 269-277.
- Lakatos PL, Kiss LS, Palatka K, Altorjay I, Antal-Szalmas P, et al. (2011) Serum lipopolysaccharide-binding protein and soluble CD14 are markers of disease activity in patients with Crohn's disease. Inflamm Bowel Dis 17: 767-777.
- Exley AR, Leese T, Holliday MP, Swann RA, Cohen J (1992) Endotoxaemia and serum tumour necrosis factor as prognostic markers in severe acute pancreatitis. Gut 33: 1126-1128.
- Bose SM, Verma GR, Mazumdar A, Giridhar M, Ganguly NK (2002) Significance of serum endotoxin and antiendotoxin antibody levels in predicting the severity of acute pancreatitis. Surg Today 32: 602-607.
- Buttenschoen K, Berger D, Hiki N, Buttenschoen DC, Vasilescu C, et al. (2000) Endotoxin and antiendotoxin antibodies in patients with acute pancreatitis. Eur J Surg 166: 459-466.
- Wig JD, Kochhar R, Ray JD, Krishna Rao DV, Gupta NM, et al. (1998) Endotoxemia predicts outcome in acute pancreatitis. J Clin Gastroenterol 26: 121-124.
- Martinez J, Palazon JM, Munoz C, Lopez M, Sanchez-Paya J, et al. (2002) Endotoxin and anti-endotoxin antibodies in the prognosis of acute pancreatitis. Rev Esp Enferm Dig 94: 406-416.
- Ammori BJ, Fitzgerald P, Hawkey P, McMahon MJ (2003) The early increase in intestinal permeability and systemic endotoxin exposure in patients with severe acute pancreatitis is not associated with systemic bacterial translocation: molecular investigation of microbial DNA in the blood. Pancreas 26: 18-22.
- Schietroma M, Pessia B, Carlei F, Mariani P, Sista F, et al. (2016) Intestinal permeability and systemic endotoxemia in patients with acute pancreatitis. Ann Ital Chir 87: 138-144.
- Deng WS, Zhang J, Ju H, Zheng HM, Wang J, et al. (2015) Arpin contributes to bacterial translocation and development of severe acute pancreatitis. World J Gastroenterol 21: 4293-4301.
- Capurso G, Zerboni G, Signoretti M, Valente R, Stigliano S, et al. (2012) Role of the gut barrier in acute pancreatitis. J Clin Gastroenterol 46 Suppl: S46-51.
- Tan C, Ling Z, Huang Y, Cao Y, Liu Q, et al. (2015) Dysbiosis of Intestinal Microbiota Associated With Inflammation Involved in the Progression of Acute Pancreatitis. Pancreas 44: 868-875.
- Bailey ME (1976) Endotoxin, bile salts and renal function in obstructive jaundice. Br J Surg 63: 774-778.
- Kimmings AN, van Deventer SJ, Obertop H, Rauws EA, Huibregtse K, et al. (2000) Endotoxin, cytokines, and endotoxin binding proteins in obstructive jaundice and after preoperative biliary drainage. Gut 46: 725-731
- Ljungdahl M, Osterberg J, Ransjo U, Engstrand L, Haglund U (2007) Inflammatory response in patients with malignant obstructive jaundice. Scand J Gastroenterol 42:94-102.
- Parks RW, Clements WD, Smye MG, Pope C, Rowlands BJ, et al. (1996) Intestinal barrier dysfunction in clinical and experimental obstructive jaundice and its reversal by internal biliary drainage. Br J Surg 83: 1345-1949.
- Welsh FK, Ramsden CW, MacLennan K, Sheridan MB, Barclay GR, et al. (1998) Increased intestinal permeability and altered mucosal immunity in cholestatic jaundice. Ann Surg 227: 205-212.
- Assimakopoulos SF, Vagianos CE, Charonis A, Nikolopoulou VN, Scopa CD (2005) Intestinal failure in obstructive jaundice. World J Gastroenterol 11: 3806-3807.
- Assimakopoulos SF, Tsamandas AC, Louvros E, Vagianos CE, Nikolopoulou VN, et al. (2011) Intestinal epithelial cell proliferation, apoptosis and expression of tight junction proteins in patients with obstructive jaundice. Eur J Clin Invest 41: 117-125.
- Niebauer J, Volk HD, Kemp M, Dominguez M, Schumann RR, et al. (1999) Endotoxin and immune activation in chronic heart failure: a prospective cohort study. Lancet 353: 1838-1842.
- Sandek A, Bjarnason I, Volk HD, Crane R, Meddings JB, et al. (2012) Studies on bacterial endotoxin and intestinal absorption function in patients with chronic heart failure. Int J Cardiol 157: 80-85.
- Sharma R, Bolger AP, Li W, Davlouros PA, Volk HD, et al. (2003) Elevated circulating levels of inflammatory cytokines and bacterial endotoxin in adults with congenital heart disease. Am J Cardiol 92: 188-193.
- Rogler G, Rosano G (2014) The heart and the gut. Eur Heart J 35: 426-430.
- Goldstein DA, Horowitz RE, Petit S, Haldimann B, Massry SG (1981) The duodenal mucosa in patients with renal failure: Response to 1,25(OH)2D3. Kidney Int 19: 324-331
- Vaziri ND, Dure-Smith B, Miller R, Mirahmadi MK (1985) Pathology of gastrointestinal tract in chronic hemodialysis patients: an autopsy study of 78 cases. Am J Gastroenterol 80: 608-611.
- Szeto CC, Kwan BC, Chow KM, Lai KB, Chung KY, et al. (2008) Endotoxemia is related to systemic inflammation and atherosclerosis in peritoneal dialysis patients. Clin J Am Soc Nephrol 3: 431-436.
- McIntyre CW, Harrison LE, Eldehni MT, Jefferies HJ, Szeto CC, et al. (2011) Circulating endotoxemia: a novel factor in systemic inflammation and cardiovascular disease in chronic kidney disease. Clin J Am Soc Nephrol 6: 133-141.
- Feroze U, Kalantar-Zadeh K, Sterling KA, Molnar MZ, Noori N, et al. (2012) Examining associations of circulating endotoxin with nutritional status, inflammation, and mortality in hemodialysis patients. J Ren Nutr 22: 317-326.
- Vaziri ND (2012) CKD impairs barrier function and alters microbial flora of the intestine: a major link to inflammation and uremic toxicity. Curr Opin Nephrol Hypertens 21: 587-92.
- Vaziri ND, Wong J, Pahl M, Piceno YM, Yuan J, et al. (2013) Chronic kidney disease alters intestinal microbial flora. Kidney Int 83: 308-815.
- Purohit V, Bode JC, Bode C, Brenner DA, Choudhry MA, et al. (2008) Alcohol, intestinal bacterial growth, intestinal permeability to endotoxin, and medical consequences: summary of a symposium. Alcohol 42: 349-361.
- Kobayashi T, Tani T, Yokota T, Kodama M (2000) Detection of peptidoglycan in human plasma using the silkworm larvae plasma test. FEMS Immunol Med Microbiol 28: 49-53.
- Tsuchiya M, Asahi N, Suzuoki F, Ashida M, Matsuura S (1996) Detection of peptidoglycan and beta-glucan with silkworm larvae plasma test. FEMS Immunol Med Microbiol 15: 129-134.
- Tabata T, Tani T, Endo Y, Hanasawa K (2002) Bacterial translocation and peptidoglycan translocation by acute ethanol administration. J Gastroenterol 37: 726-731.
- Shimizu T, Tani T, Endo Y, Hanasawa K, Tsuchiya M (2002) Elevation of plasma peptidoglycan and peripheral blood neutrophil activation during hemorrhagic shock: plasma peptidoglycan reflects bacterial translocation and may affect neutrophil activation. Crit Care Med 30: 77-82.
- Shimizu T, Endo Y, Tabata T, Mori T, Hanasawa K (2005) Diagnostic and predictive value of the silkworm larvae plasma test for postoperative infection following gastrointestinal surgery. Crit Care Med 33: 1288-1295.
- Tsunooka N, Maeyama K, Hamada Y, Imagawa H, Takano S (2004) Bacterial translocation secondary to small intestinal mucosal ischemia during cardiopulmonary bypass. Measurement by diamine oxidase and peptidoglycan. Eur J Cardiothorac Surg 25: 275-280.
- Kim OY, Monsel A, Bertrand M, Cavaillon JM, Coriat P (2009) Translocation of bacterial NOD2 agonist and its link with inflammation. Crit Care 13: 124.
- Cole CR, Frem JC, Schmotzer B, Gewirtz AT, Meddings JB, et al (2010) The rate of bloodstream infection is high in infants with short bowel syndrome: relationship with small bowel bacterial overgrowth, enteral feeding, and inflammatory and immune responses. J Pediatr 156: 941-957.
- Ziegler TR, Luo M, Estivariz CF, Moore DA, Sitaraman SV, et al. (2008) Detectable serum flagellin and lipopolysaccharide and upregulated anti-flagellin and lipopolysaccharide immunoglobulins in human short bowel syndrome. Am J Physiol Regul Integr Comp Physiol 294.
- Gewirtz AT, Navas TA, Lyons S, Godowski PJ, Madara JL (2001) Cutting edge: bacterial flagellin activates basolaterally expressed TLR5 to induce epithelial proinflammatory gene expression. J Immunol 167: 1882-1885.
- Lodes MJ, Cong Y, Elson CO, Mohamath R, Landers CJ, Targan SR, Fort M, Hershberg RM. Bacterial flagellin is a dominant antigen in Crohn disease. J Clin Invest 113: 1296-306.
- Sitaraman SV, Klapproth JM, Moore DA, Landers C, Targan S (2005) Elevated flagellin-specific immunoglobulins in Crohn's disease. Am J Physiol Gastrointest Liver Physiol 288: 403-406,
- Targan SR, Landers CJ, Yang H, Lodes MJ, Cong Y (2005) Antibodies to CBir1 flagellin define a unique response that is associated independently with complicated Crohn's disease. Gastroenterology 128: 2020-2028.
- Dlugosz A, Nowak P, D'Amato M, Kermani MG (2015) Increased serum levels of lipopolysaccharide and antiflagellin antibodies in patients with diarrhea-predominant irritable bowel syndrome. Neurogastroenterol Motil 27: 1747-1754.
- Brenchley JM, Price DA, Schacker TW, Asher TE, Silvestri G, et al. (2006) Microbial translocation is a cause of systemic immune activation in chronic HIV infection. Nat Med 12: 1365-1371.
- Paiardini M, Frank I, Pandrea I, Apetrei C, Silvestri G (2008) Mucosal immune dysfunction in AIDS pathogenesis. AIDS Rev 10: 36-46.
- Vesterbacka J, Nowak P, Barqasho B, Abdurahman S, Nystrom J (2013) Kinetics of microbial translocation markers in patients on efavirenz or lopinavir/r based antiretroviral therapy. PLoS One 8: e55038.
- Munukka E, Wiklund P, Partanen T, Valimaki S, Laakkonen EK, et al. (2016) Adipocytes as a link between gut microbiota-derived flagellin and hepatocyte fat accumulation. PLoS One 11: e0152786.
- Finney SJ, Leaver SK, Evans TW, Burke-Gaffney A (2012) Differences in lipopolysaccharide- and lipoteichoic acid-induced cytokine/chemokine expression. Intensive Care Med 38: 324-332.
- Haddadi S, Thapa S, Kameka AM, Hui J, Czub M, et al. (2015) Toll-like receptor 2 ligand, lipoteichoic acid is inhibitory against infectious laryngotracheitis virus infection in vitro and in vivo. Dev Comp Immunol 48: 22-32.
- van Langevelde P, van Dissel JT, Ravensbergen E, Appelmelk BJ, Schrijver IA, et al. (1998) Antibiotic-induced release of lipoteichoic acid and peptidoglycan from Staphylococcus aureus: quantitative measurements and biological reactivities. Antimicrob Agents Chemother 42: 3073-3078.
- Levels JH, Abraham PR, van Barreveld EP, Meijers JC, van Deventer SJ (2003) Distribution and kinetics of lipoprotein-bound lipoteichoic acid. Infect Immun 71: 3280-4. 155762.
- Tsuneyama K, Harada K, Kono N, Hiramatsu K, Zen Y, et al. (2001) Scavenger cells with gram-positive bacterial lipoteichoic acid infiltrate around the damaged interlobular bile ducts of primary biliary cirrhosis. J Hepatol 35: 156-163.
- Haruta I, Hashimoto E, Kato Y, Kikuchi K, Kato H (2006) Lipoteichoic acid may affect the pathogenesis of bile duct damage in primary biliary cirrhosis. Autoimmunity 39: 129-35.
- Morris A, Hillenbrand M, Finkelman M, George MP, Singh V, et al. (2012) Serum (1-->3)-beta-D-glucan levels in HIV-infected individuals are associated with immunosuppression, inflammation, and cardiopulmonary function. J Acquir Immune Defic Syndr 61: 462-468.
- Kikkert R, Bulder I, de Groot ER, Aarden LA, Finkelman MA (2007). Potentiation of Toll-like receptor-induced cytokine production by (1-->3)-beta-D-glucans: implications for the monocyte activation test. J Endotoxin Res13: 140-149.
- Hoenigl M, Oliveira MF, Perez-Santiago J, Zhang Y, Morris S (2016) (1-->3)-beta-D-Glucan Levels Correlate With Neurocognitive Functioning in HIV-Infected Persons on Suppressive Antiretroviral Therapy: A Cohort Study. Medicine (Baltimore) 95: e3162.
- Guo Y, Zhou G, He C, Yang W, He Z (2015) Serum Levels of Lipopolysaccharide and 1,3-beta-D-Glucan Refer to the Severity in Patients with Crohn's Disease. Mediators Inflamm 2015: 843089.
- Kane TD, Alexander JW, Johannigman JA (1998) The detection of microbial DNA in the blood: a sensitive method for diagnosing bacteremia and/or bacterial translocation in surgical patients. Ann Surg 227:1-9.
- Vaishnavi C (2013) Translocation of gut flora and its role in sepsis. Indian J Med Microbiol 31: 334-342.
- Rutz M, Metzger J, Gellert T, Luppa P, Lipford GB, (2004) Toll-like receptor 9 binds single-stranded CpG-DNA in a sequence- and pH-dependent manner. Eur J Immunol 34: 2541-2550.
- Mortensen C, Karlsen S, Gronbaek H, Nielsen DT, Frevert S (2013) No difference in portal and hepatic venous bacterial DNA in patients with cirrhosis undergoing transjugular intrahepatic portosystemic shunt insertion. Liver Int 33: 1309-1315
- Frances R, Gonzalez-Navajas JM, Zapater P, Munoz C, Cano R (2007) Translocation of bacterial DNA from Gram-positive microorganisms is associated with a species-specific inflammatory response in serum and ascitic fluid of patients with cirrhosis. Clin Exp Immunol 150: 230-237.
- Bellot P, Garcia-Pagan JC, Frances R, Abraldes JG, Navasa M, et al. (2010) Bacterial DNA translocation is associated with systemic circulatory abnormalities and intrahepatic endothelial dysfunction in patients with cirrhosis. Hepatology 52: 2044-2052.
- Gonzalez-Navajas JM, Bellot P, Frances R, Zapater P, Munoz C, et al. (2008) Presence of bacterial-DNA in cirrhosis identifies a subgroup of patients with marked inflammatory response not related to endotoxin. J Hepatol 48: 61-67.
- Ortiz S, Zapater P, Estrada JL, Enriquez P, Rey M (2014) Bacterial DNA translocation holds increased insulin resistance and systemic inflammatory levels in morbid obese patients. J Clin Endocrinol Metab 99: 2575-2583.
- Gutierrez A, Scharl M, Sempere L, Holler E, Zapater P (2014) Genetic susceptibility to increased bacterial translocation influences the response to biological therapy in patients with Crohn's disease. Gut 63: 272-280
- Li Y, Zuo L, Zhu W, Gong J, Zhang W (2015) The impact of bacterial DNA translocation on early postoperative outcomes in Crohn's patients undergoing abdominal surgery. J Crohns Colitis 9: 259-265.
- Szeto CC, Kwan BC, Chow KM, Kwok JS, Lai KB, et al. (2015) Circulating bacterial-derived DNA fragment level is a strong predictor of cardiovascular disease in peritoneal dialysis patients. PLoS One 10: e0125162.
- Kwan BC, Chow KM, Leung CB, Law MC, Cheng PM (2013) Circulating bacterial-derived DNA fragments as a marker of systemic inflammation in peritoneal dialysis. Nephrol Dial Transplant 28: 2139-2145.
- Bossola M, Sanguinetti M, Scribano D, Zuppi C, Giungi S, (2009) Circulating bacterial-derived DNA fragments and markers of inflammation in chronic hemodialysis patients. Clin J Am Soc Nephrol 4: 379-385.
- Garcia-Alvarez M, Berenguer J, Guzman-Fulgencio M, Alvarez E, Cosin J (2012) Bacterial DNA translocation and liver disease severity among HIV-infected patients with chronic hepatitis C. J Acquir Immune Defic Syndr 61: 552-556.
- Bala S, Marcos M, Gattu A, Catalano D, Szabo G (2014) Acute binge drinking increases serum endotoxin and bacterial DNA levels in healthy individuals. PLoS One 9: e96864.
- Kanuri G, Ladurner R, Skibovskaya J, Spruss A, Konigsrainer A (2015) Expression of toll-like receptors 1-5 but not TLR 6-10 is elevated in livers of patients with non-alcoholic fatty liver disease. Liver Int 35: 562-568.
- Szabo G (2015) Gut-liver axis in alcoholic liver disease. Gastroenterology 148: 30-36.
- Starkel P, de Saeger C, Strain AJ, Leclercq I, Horsmans Y (2010) TLR 3 and 7 expression in human end-stage HCV and alcoholic liver disease. Eur J Clin Invest 40: 575-584.
- Gustot T, Lemmers A, Moreno C, Nagy N, Quertinmont E, et al. (2006) Differential liver sensitization to toll-like receptor pathways in mice with alcoholic fatty liver. Hepatology 43: 989-1000.
- Yang L, Seki E (2012) Toll-like receptors in liver fibrosis: cellular crosstalk and mechanisms. Front Physiol 3: 138.
- Lian JQ, Wang XQ, Zhang Y, Huang CX, Bai XF (2009) Correlation of circulating TLR2/4 expression with CD3+/4+/8+ T cells and Treg cells in HBV-related liver cirrhosis. Viral Immunol 22: 301-308.
- Manigold T, Bocker U, Hanck C, Gundt J, Traber P, et al. (2003) Differential expression of toll-like receptors 2 and 4 in patients with liver cirrhosis. Eur J Gastroenterol Hepatol 15: 275-282.
- Riordan SM, Skinner N, Nagree A, McCallum H, McIver CJ, et al. (2003) Peripheral blood mononuclear cell expression of toll-like receptors and relation to cytokine levels in cirrhosis. Hepatology 37: 1154-1164.
- Tazi KA, Quioc JJ, Saada V, Bezeaud A, Lebrec D, et al. (2006) Upregulation of TNF-alpha production signaling pathways in monocytes from patients with advanced cirrhosis: possible role of Akt and IRAK-M. J Hepatol 45: 280-289.
- Testro AG, Gow PJ, Angus PW, Wongseelashote S, Skinner N, et al. (2010) Effects of antibiotics on expression and function of Toll-like receptors 2 and 4 on mononuclear cells in patients with advanced cirrhosis. J Hepatol 52: 199-205,
- Soares JB, Pimentel-Nunes P, Afonso L, Rolanda C, Lopes P, et al. (2012) Increased hepatic expression of TLR2 and TLR4 in the hepatic inflammation-fibrosis-carcinoma sequence. Innate Immun 18: 700-708.
- Takii Y, Nakamura M, Ito M, Yokoyama T, Komori A, et al. (2005) Enhanced expression of type I interferon and toll-like receptor-3 in primary biliary cirrhosis. Lab Invest 85: 908-920.
- Honda Y, Yamagiwa S, Matsuda Y, Takamura M, Ichida T, et al. (2007) Altered expression of TLR homolog RP105 on monocytes hypersensitive to LPS in patients with primary biliary cirrhosis. J Hepatol 47: 404-411.
- Brown M, Hughes KR, Moossavi S, Robins A, Mahida YR (2014) Toll-like receptor expression in crypt epithelial cells, putative stem cells and intestinal myofibroblasts isolated from controls and patients with inflammatory bowel disease. Clin Exp Immunol 178: 28-39.
- Dasu MR, Devaraj S, Park S, Jialal I (2010) Increased toll-like receptor (TLR) activation and TLR ligands in recently diagnosed type 2 diabetic subjects. Diabetes Care 33: 861-868.
- Dasu MR, Martin SJ (2014) Toll-like receptor expression and signaling in human diabetic wounds. World J Diabetes 5: 219-223.
- Lin M, Tang SC (2014) Toll-like receptors: Sensing and reacting to diabetic injury in the kidney. Nephrol Dial Transplant 29: 746-754.
- Yiu WH, Lin M, Tang SC (2014) Toll-like receptor activation: from renal inflammation to fibrosis. Kidney Int Suppl 4: 20-25.
- Lester RT, Yao XD, Ball TB, McKinnon LR, Kaul R, et al. (2008) Toll-like receptor expression and responsiveness are increased in viraemic HIV-1 infection. AIDS 22: 685-694.
- Pandey GN, Rizavi HS, Ren X, Bhaumik R, Dwivedi Y (2014) Toll-like receptors in the depressed and suicide brain. J Psychiatr Res 53: 62-68.
- Hadley JS, Wang JE, Michaels LC, Dempsey CM, Foster SJ, et al. (2007) Alterations in inflammatory capacity and TLR expression on monocytes and neutrophils after cardiopulmonary bypass. Shock 27: 466-473.
- Rice PJ, Adams EL, Ozment-Skelton T, Gonzalez AJ, Goldman MP (2005) Oral delivery and gastrointestinal absorption of soluble glucans stimulate increased resistance to infectious challenge. J Pharmacol Exp Ther 314: 1079-1086.
- Marshall JC, Walker PM, Foster DM, Harris D, Ribeiro M, et al. (2002) Measurement of endotoxin activity in critically ill patients using whole blood neutrophil dependent chemiluminescence. Crit Care 6: 342-348.
- Yaroustovsky M, Plyushch M, Popov D, Samsonova N, Abramyan M, et al. (2013) Prognostic value of endotoxin activity assay in patients with severe sepsis after cardiac surgery. J Inflamm (Lond) 10: 8.
- Ikeda T, Ikeda K, Suda S, Ueno T (2014) Usefulness of the endotoxin activity assay as a biomarker to assess the severity of endotoxemia in critically ill patients. Innate Immun 20: 881-887.
- Sakamoto Y, Inoue S, Iwamura T, Yamashita T, Nakashima A (2014) Usefulness of the endotoxin activity assay to evaluate the degree of lung injury. Yonsei Med J 55: 975-979.
- Sanada Y, Urahashi T, Ihara Y, Okada N, Yamada N, et al. (2014) pretransplant levels of endotoxin can predict the risk of bacterial infections and graft liver function after liver transplantation. Eur J Pediatr Surg 2014;10.
- Ding JL, Ho B (2010) Endotoxin detection--from limulus amebocyte lysate to recombinant factor C. Subcell Biochem 53:187-208.
- Zuzuarregui A, Souto D, Perez-Lorenzo E, Arizti F, Sanchez-Gomez S, et al. (2015) Novel integrated and portable endotoxin detection system based on an electrochemical biosensor. Analyst 140: 654-660.
- Jiang H, Jiang D, Shao J, Sun X, Wang J (2016) High-throughput living cell-based optical biosensor for detection of bacterial lipopolysaccharide (LPS) using a red fluorescent protein reporter system. Sci Rep 6: 36987.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences